
May 2006, strolling along the sun-kissed shores of the Indian Ocean, having spent 16 glorious days on the beautiful island of Mauritius, I turned to my partner, John. No longer could I keep the secret that I had been saving for the “right moment” and announced that we had a much longed for baby on the way. This news was the icing on the cake for what had been a wonderful year for us as a couple and now we had a bright future to look forward to with a child of our own. We returned to Ireland filled with excitement and looking forward to the pregnancy and our new roles as parents. For the next nine weeks my pregnancy was a mixture of day long “morning sickness” followed by periods of extreme fatigue, but nothing could dampen the joy and love that we felt for our growing infant.

Suddenly, without warning at week 13, just hours after I publicly announced my pregnancy to family, friends and work colleagues, our world fell apart. I began to hemorrhage and was admitted to the Emergency Room of our Maternity Hospital (a place I never knew existed) with a suspected miscarriage. Thankfully, my pregnancy was still intact, but from that moment on, a cloud of uncertainty and trepidation robbed me of my inner happiness. My unpredictable pregnancy journey would chip away at my mental well-being and self-esteem. I continued to bleed and our trips to the ER would become an all too regular occurrence. Insomnia filled my nights as the grip of fear embraced every waking minute of my days. For the subsequent 12 weeks, I opted for bed-rest, hoping beyond hope that this pregnancy would continue to the point whereby my medical team would intervene to save my infant’s life if he or she decided to arrive early. No longer could I plan for the future; surviving each day was a challenge and I wished that I could simply fall asleep and wake up at week 24. Nothing prepared me for the painful isolation, the uncontrollable fear and the heart-shattering loneliness that became the mainstay of my pregnancy; I felt adrift on a stormy sea and every day I could see a part of me dying inside.
What I needed most was for someone to take me in their arms and offer me the emotional support and reassurance that I needed to help me reach my goal of 24 weeks. However, the reality was an abyss that I had to navigate alone and against a tide of a system whereby the welfare of the mother-to-be was not valued unless she had reached 24 weeks gestation. How would I find the mental strength to continue and what long-term effect would this journey have on us as a couple and on our future family life?
My one glimmer of hope lay with a young female doctor who quietly offered me weekly ante-natal appointments and scans (going against hospital protocol). I lived for the two hour journey to the hospital every Tuesday morning and the elation and joy that I felt on each occasion that I had the opportunity to see my unborn daughter on the ultrasound scan.
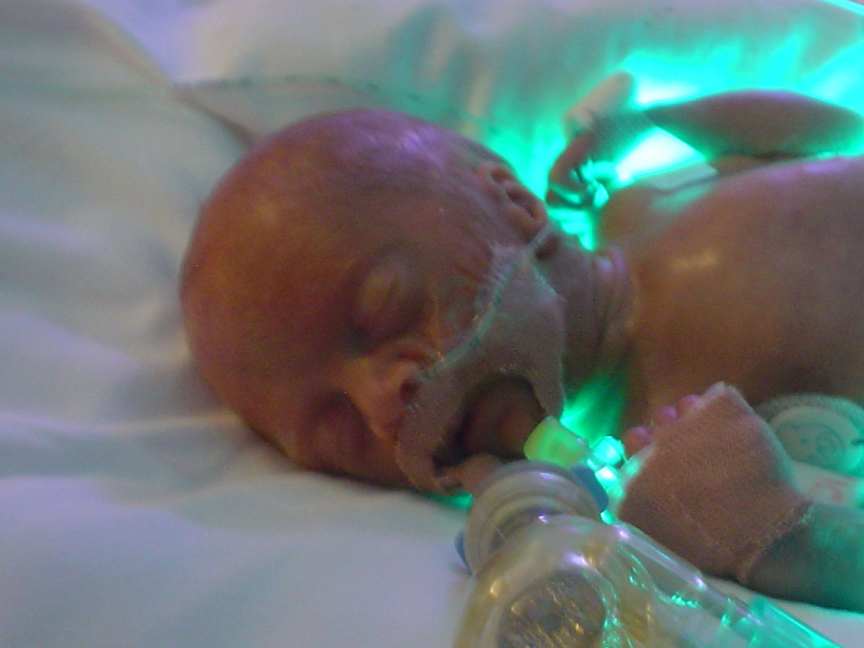
At 25 weeks and 6 days into my pregnancy things started to take a turn for the worse. Despite going to the ER, I was sent home without having antenatal steroids administered: a crucial factor that would change the course of our lives. Within a few short hours I had suffered a placental abruption and had travelled 160 miles to reach a tertiary hospital that had the expertise to offer my daughter the best possible chance of life. Amelia Faith was delivered by emergency caesarean section at 4:35A.M. on Sunday October 8, 2006 weighing 780 grams (1.7 pounds). My memories of her birth are of a room filled with strangers, some assigned to save my life and others assigned to Amelia who required resuscitation for nine minutes. One could smell the uncertainty in the room, no-one spoke and life stood still for me as I lay on the table not knowing if either of us would survive. I missed that wonderful birth moment when the parents get to touch, smell and hold their infant; in contrast I could hear the frantic efforts in the corner of the room desperately breathing life into my little girl. My partner was escorted from the room to accompany the team as they transported our daughter to the Neonatal Intensive Care Unit as I closed my eyes and for a brief time allowed my body and mind to rest; not knowing if I would wake again and if I did….what awaited me.
I woke to find myself sharing a room with five other new mothers, all of whom had their newborn infants in cots next to their beds. My heart had been ripped out a few short hours earlier, but nothing could have prepared me for the depth of sadness that I would feel as I heard these infants crying and watched their proud and joyful mothers feed them. Drawing the curtains around my bed, I curled up under the blankets and cried more deeply than I had ever done in my life. Grief overwhelmed me…I had lost my pregnancy, my birth, my hopes for the future and I had nearly lost my life.
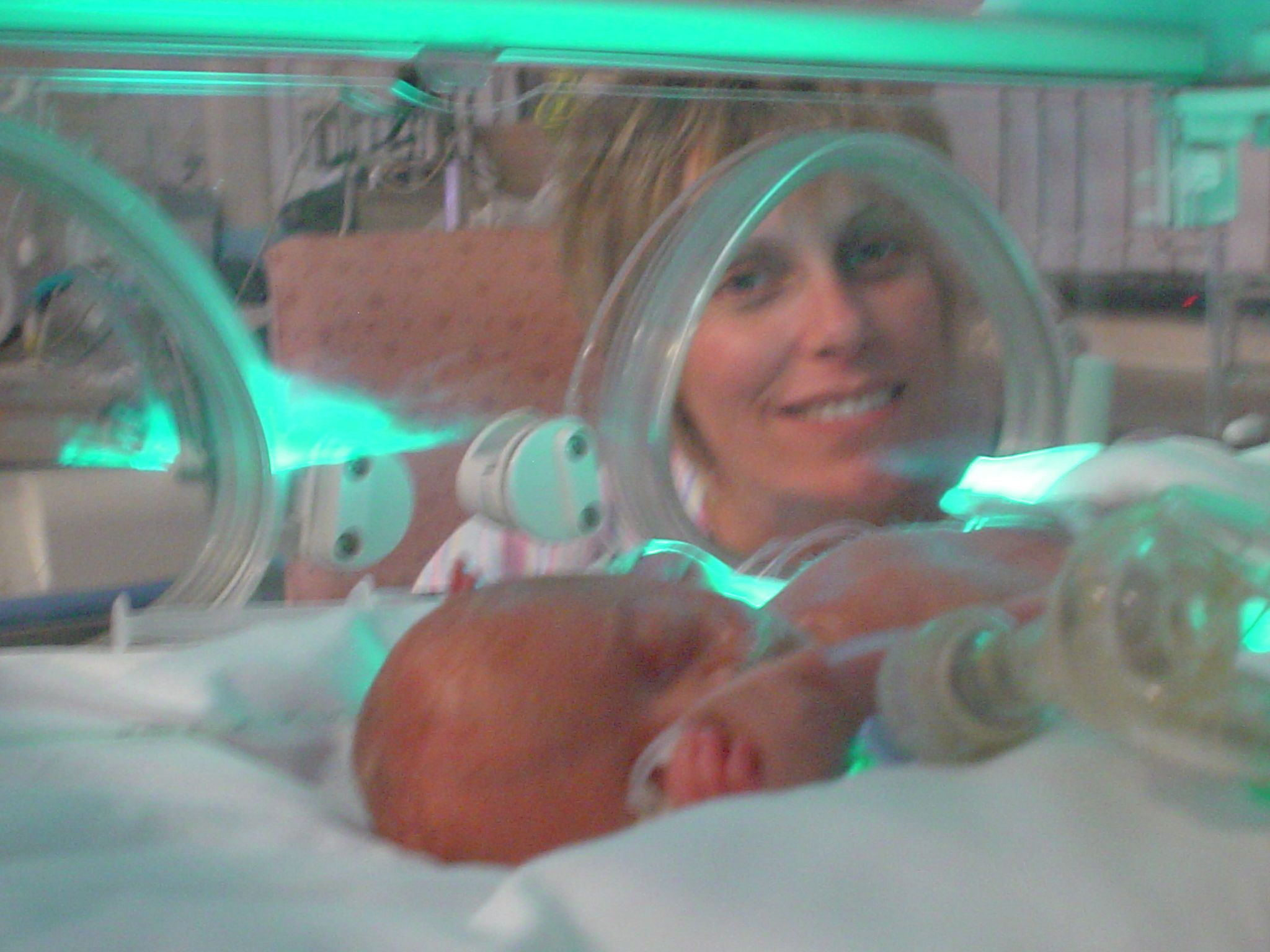
Twelve hours post-delivery, I was wheeled towards this place called the NICU to meet my daughter. The long, sterile corridor from the lift to the locked doors of the NICU, doors upon which were listed more rules than I was capable of reading, would become that walk of fear for me for many months to come. The swishing of the lift doors heralded an increase in anxiety as each step towards the NICU flooded my mind with the countless possibilities that would await me once I had been granted admission to the NICU to visit my child. Staring numbly through the glass windows that separated the hand-washing area from the NICU, I was prepared to accept any one of the ten infants who were fighting for their tiny lives in the incubators. It struck me I had no idea what my daughter looked like despite being over 12 hours old, a fact that eroded my ever flagging confidence as a new mother. Meeting Amelia for the first time should have filled my heart with love, but what lay before me was a skeletal little human, who barely resembled any new baby that I had ever seen and for whom medical technology appeared to be performing every little task of living. Her eyes were still fused, her skin translucent and her body was still covered in lanugo. I couldn’t bring myself to open the door of the incubator to touch Amelia, such was my fear of exacerbating an already fragile situation for both my daughter and myself.
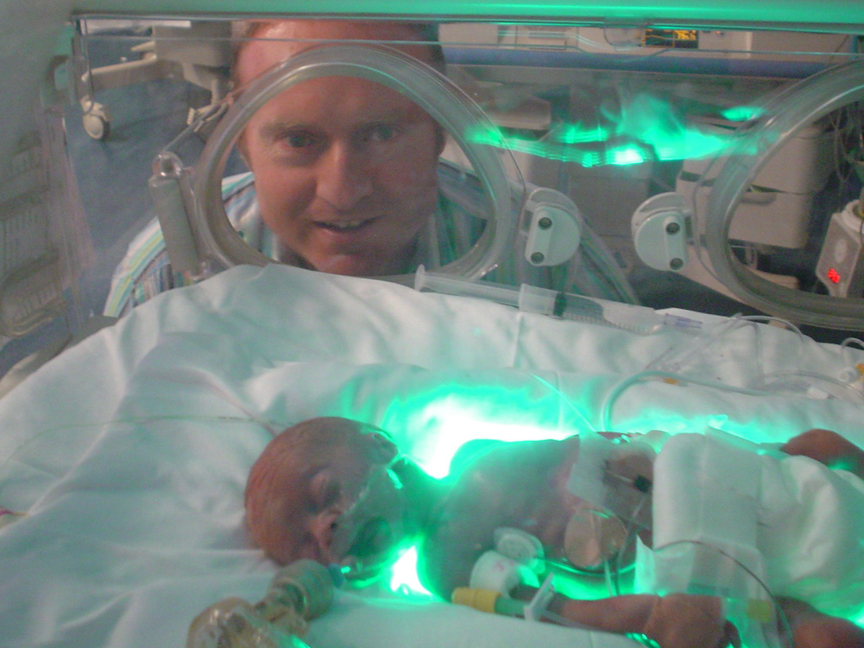
Life has an uncanny way of throwing unexpected life-lines, as the neonatologist assigned to Amelia can only be described as an angel in disguise sent to protect and care for our family. Not only did she see Amelia as her patient, but from the outset, she embraced me and my partner, John as her patients, friends and fellow parents too. She was a pioneer in the unit by virtue of her understanding of the trauma suffered by the family and she did everything in her power to help the families heal; but she was a lone crusader in her quest.
As one tumultuous journey came to an end for us on October 8, 2006, another journey of getting to know our daughter in the clinical surroundings of the NICU began. The three of us had physically survived the high-risk pregnancy and the life and death delivery. Our mental well-being was an entirely different story, one that would continue to unfold for many years.
Mandy C. Daly, Dip. H Diet & Nutrition, Dip. Ki Massage, ACII, DLDU
Director of Advocacy & Policy Making, Irish Neonatal Health Alliance
Parent Advisory Board Member, European Foundation for the Care of Newborn Infants
Board Member, NIDCAP Federation International