
It was September 7, 2003 and I had been on bed rest for a little over a day. The day before I had been in a car coming back from an extended family outing when I felt my bladder let go in the front seat. Embarrassed, I said nothing, but quietly asked my husband, Gregg, to get to the nearest bathroom. All alone in a grocery store bathroom, I discovered that my water had broken. With tears streaming down my face, I apologized to my daughter in quiet hysterics and then frantically called family members in the car only to get voicemail after voicemail message. So I cleaned up as best I could and headed to the front of the store, stopping in at the office and in a surreally calm voice relayed and asked, “I believe I am in preterm labor. Where is the nearest hospital? May I borrow your phone to call my doctor?” The two ladies in the office picked up their collective jaws off the floor and at my direction ran to get my husband as I prepared to leave a message with the doctor’s answering service. As I did so and as my husband and my brother in-law rushed into the office, my mind flitted back to a month prior when I had told my OB of my concern that I would deliver early. “Oh no, this is your first baby so you will be late.” Uh-huh, late indeed.
My husband drove like a true father-to-be in full-on maniac mode heading us to the hospital in 45 minutes when it really should have taken over an hour. After 30 hours of poking, bed rest, medications, oxygen, drugs that I wouldn’t give to my worst enemy and medications to mature my unborn daughter’s lungs, my body couldn’t hold back anymore and I delivered my daughter at 11:50 p.m. on Grandparents Day. She came at 30 weeks gestation and weighed 2 lbs. 15.5 oz. and let out the tiniest but most fierce cry. I was beyond grateful to hear that sound because we weren’t sure if she would even be able to do that. The room erupted in a unified joyful “Ohhhhhhh!” and my husband both laughed and cried. I silently thanked God for this miracle and for the wonderful nurse who held my daughter up to me to see before the team whisked her away to the NICU along with my husband.
But nothing prepared me for the shock I felt seeing my daughter in the NICU, nor the helplessness of watching her struggle on the warming table and later inside the incubator. I wanted to hide in my room and wish away this awful nightmare. Where was that instant mother-infant connection so many people had told me about? I felt like I didn’t belong there as I watched medical team members attend to my daughter’s every need while I was told to touch her through the portholes of the incubator for a tiny bit and then take her temperature. That was not parenting. I soon learned that parenting was something that often gets shoved aside in the NICU, left to be nurtured when the infant is deemed more medically stable.
I didn’t know it at the time, but I was quickly gaining my parenting instinct and my Preemie Mom instinct, too. Within eight hours of giving birth I was staring at the breast pump in my postpartum room. “I should be trying to pump breast milk, Gregg,” I noted, quickly realizing my daughter would need that at one point to help with proper nutrition. I can say, without any doubt, that my first time with a breast pump was comical. Later I realized I was doing everything wrong, but hey, some yellow stuff came out and I told Gregg to go ask the nurse if it was even worth keeping. Gregg came back into my room with an ear-splitting grin on his face saying, “The nurse is rushing it down to the NICU right now. She said this is Liquid Gold!” No one had said a word to me. No one had suggested it. Yet this stuff is gold?
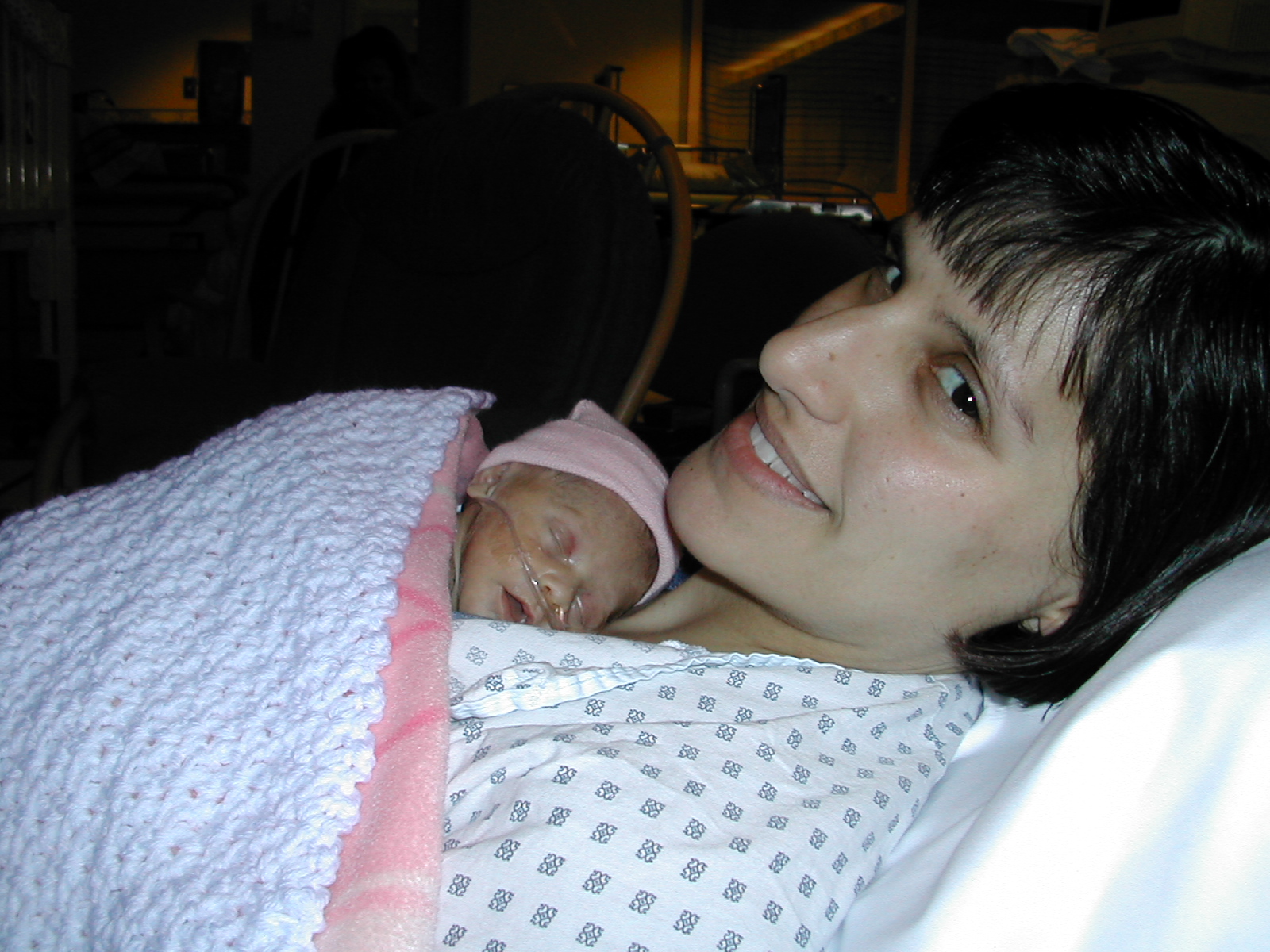
My in-laws arrived the day after the birth and at one point in their visit, my mother in-law wondered aloud when I would be allowed to do something called “Kangaroo Care.” I made it my mission to ask about this at the NICU as soon as Becky was deemed stable enough to hold. One day I clearly stated that I wanted to do Kangaroo Care even though I had no clue what it was. Where is this kangaroo everyone keeps talking about? And how does it help my daughter? A special type of lounge chair was brought out and I was asked to undo the buttons to my shirt. Next thing I knew I felt like I was being thrown backward to the point of falling out of the chair and then my daughter, in just a diaper, was placed on my chest. It was surreal. My daughter felt like a cold, crawling insect on my chest. Some mother I am! Then Gregg kept telling me that I just had to see the look on Becky’s face. Take pictures, get me a mirror, because I can’t see from this angle! When he showed me the pictures, I was stunned. She was so peaceful. I found myself glancing at her monitors and wondering if this was stressing her or not. Wow, she is stabilizing! I made a point of doing Kangaroo Care as much as was allowable. With my crazy schedule it was hard but we did get Kangaroo Care time in as regularly as possible.

A few weeks later I finally got a chance to bathe my daughter for the first time. It was scary and yet amazing all rolled up into one simple experience. But for me, it was the first time I saw my daughter naked and wireless. To me, that helped re-write some of the pain and guilt. For me, the NICU Nurse who was teaching me helped me re-do my chaotic birth experience into one of holding my fully naked newborn daughter in a moment of wonder and joy. As I scrubbed her down, I did a little massage and she responded. Hm, massage could be a good thing for her. Maybe I should figure out how to do that. Weeks later, after Becky was home, we would bathe her all of the time and I would spend the time after the bath massaging her with baby oil. She loved it and I felt it not only helped the bonding process post-NICU, but it made a difference for my daughter in a variety of developmental ways such as sleep, growth, mood and overall development itself.

As I support families today, I convey to them that parents are key team members in the NICU and that their concerns should be heard, and that they should be involved with their baby’s care as early as possible, even if it is just singing a soft lullaby or gently reading a book. They knew that baby first and that baby is best comforted by them. Parents are trying to protect and nurture their newborn as any good parent would do and medical equipment and professionals should not be a barrier to this.
I also alert families to the importance of creating a safe and comfortable environment for their infant in the NICU. What NIDCAP professionals are doing to ensure proper environmental practices in NICUs worldwide is based on real science of infant outcomes and on pure common sense. Why, after spending a huge amount of money on the best medicine possible for your infant, would you then want to have an environment working against that in terms of long-term outcomes of development? Common sense should prevail.

Deb Discenza is the mother to Becky, born at 30 weeks after conception, and now almost 12 years old, who is healthy and recognized twice as exceptional in terms of giftedness and developmental disabilities. Deb is the head of PreemieWorld (www.PreemieWorld.com) and the co-author of “The Preemie Parent’s Survival Guide to the NICU” and the originator and moderator of the free Preemie Support forum on Inspire.com at www.Inspire.com/preemie