Being With You Is Everything: Discovering Your Baby’s Voice
Four of my seven children, a son and three daughters, came home to our family through the foster system here in Massachusetts. They were...
Categories

Four of my seven children, a son and three daughters, came home to our family through the foster system here in Massachusetts. They were...

Professional trajectories are often shaped by a confluence of personal experiences, societal structures, and professional aspirations. While traditional career development frameworks emphasize strategic planning...
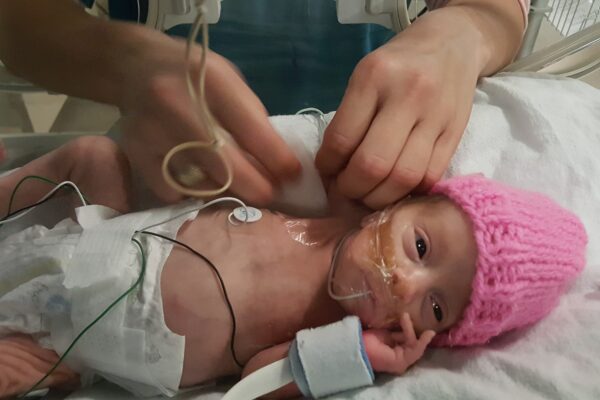
My daughter was born 5 years ago at the Meir Medical Center in Kfar Saba, Israel. She was almost 4 months premature, at 26...
Supporting breastfeeding has always been a top priority in our NICU at Meir Medical Center in Kfar-Saba, Israel. We are lucky enough to have...

Along the entrance corridor to our NICU, flat television screens show colorful pictures of our premature babies, as NICU patients and graduates of all...

There is a special job in the NICU that is “Family Support Specialist.” This person has the opportunity to walk alongside families through their...

When they announced 2020 as the Year of the Nurse and Midwife, as a nurse I felt honoured and humbled to be recognised by...

On March 20th, the NIDCAP Federation International (NFI) celebrated the 2nd Annual World NIDCAP Day. The celebrations will continue all month long. How we...

University College Hospital, London, UK is the home of the UK NIDCAP Centre. This week sees us busy with preparations to celebrate World Prematurity...

Part 2. My Impressions as a “Young” NICU Nurse In Hebrew, a new nurse in a unit or ward is often called a “young”...

Part 1. My reflections as a veteran nurse on the evolution of NIDCAP Care in our NICU I retired from work recently. I started...

I joined the NIDCAP Federation International in 2017 after attending their annual NIDCAP Trainers Meeting in Edmonton, Canada. NIDCAP stands for Newborn Individualized Developmental...

Admission to the neonatal unit occurs during a sensitive period of development. The first 1,000 days of life from conception to age three is...

Just 7 days earlier, I had an OBGYN visit. After a great visit, I asked other moms of multiples if they thought I would...

Tuve la oportunidad de tener a mis trillizos en el año 1999 en Londres, Inglaterra. Nacieron de 29 semanas de gestación en el Hospital...